Back to ALL Research Publications
![]()
![]()
![]()
![]()
![]()
 PUBLICATION_
PUBLICATION_ 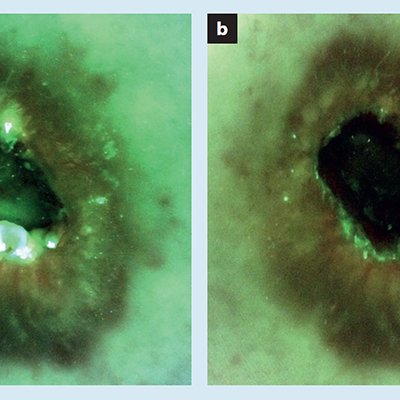 PUBLICATION_
PUBLICATION_ 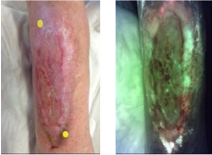 PUBLICATION_
PUBLICATION_ 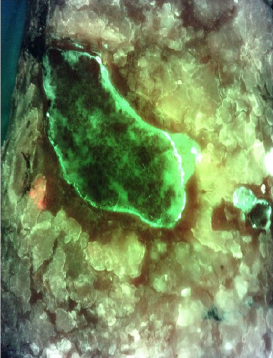 PUBLICATION_
PUBLICATION_
Research Category: ,
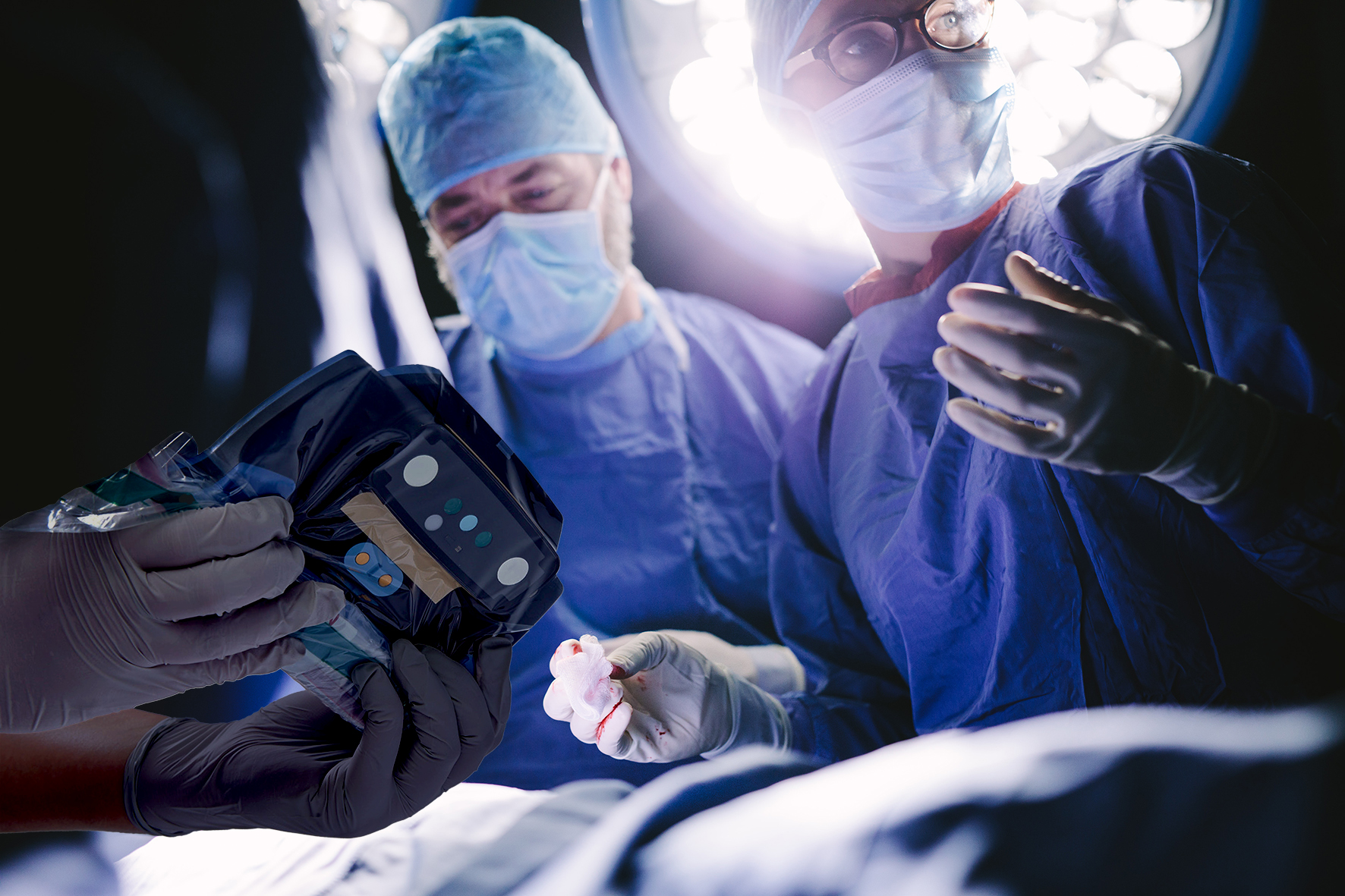
Use of a bacterial fluorescence imaging device: wound measurement, bacterial detection, and targeted debridement
Related Publications
Related Material
 PUBLICATION_
PUBLICATION_ Bacterial fluorescence imaging as a predictor of skin graft integration in burn wounds
 PUBLICATION_
PUBLICATION_ A novel debridement device for the treatment of hard-to-heal wounds: a prospective trial
 PUBLICATION_
PUBLICATION_ The Role of Autoflorescence Imaging Device in the Evaluation of Bacteria Burden Control
 PUBLICATION_
PUBLICATION_ Fluorescence-Based Evaluation of Bacterial Load in Perilesional Skin: A Comparison Between Short Stretch Bandage and Zinc Oxide Bandage
MolecuLight Headquarters
425 University Avenue Suite 700 Toronto, ON M5G 1T6 Canada
US Address MolecuLight Corp. 2403 Sidney Street, Suite 286 Pittsburgh, PA 15203
General Inquiries:
1-877-818-4360 (Toll Free)
Support:
1-833-761-0177 (Toll Free)
Fax: +1 647-362-4730
Email: info@moleculight.com
©2026
The MolecuLight® i:X and MolecuLightDX™ Imaging Devices are approved by Health Canada for sale in Canada and has CE marking for sale in the European Union.
The MolecuLight™ i:X and DX Imaging Devices have received FDA clearance.










